Digital Claims Processing: How Evidence Management Cuts Investigation Time
By Rafay Muneer on March 18, 2026, ref:

Insurance claims investigations generate an enormous volume of multimedia evidence. Loss adjustment videos, recorded policyholder statements, surveillance footage, medical records, and photos all flow into a single claim file. When adjusters manage this evidence across disconnected systems, files get lost, reviews take longer, and fraud slips through the cracks.
The shift to digital claims processing changes how insurers handle evidence from intake to resolution. Instead of scattered email attachments, shared drives, and physical media, a centralized digital workflow gives claims teams a single place to store, search, review, and share every piece of evidence tied to a claim. According to the McKinsey Global Insurance Report, insurers that digitize claims operations reduce processing time by 30 to 50 percent while improving fraud detection rates. Building a strong digital audit trail is central to making that speed gain possible.
This guide breaks down what digital claims processing actually involves, why evidence management is the missing piece for most carriers, and how to evaluate platforms that handle the full claims evidence lifecycle.
Key Takeaways
- Digital claims processing centralizes multimedia evidence (video, audio, documents, images) in a single searchable repository, cutting adjuster review time by 30% or more.
- AI-powered transcription and search let adjusters find specific statements across thousands of recorded interviews in seconds instead of hours.
- Automated PII, PCI, and PHI redaction eliminates the manual bottleneck before evidence is shared with third parties or legal teams.
- Tamper detection and full audit trails protect evidence integrity for litigation and regulatory compliance.
- Secure, time-limited sharing links replace email attachments, reducing data exposure and maintaining chain of custody.
What Is Digital Claims Processing and Why Does It Matter?
Digital claims processing is the practice of managing all claims-related evidence, communications, and workflows through electronic systems rather than paper-based or manual processes. It covers everything from first notice of loss through investigation, decision, and settlement.
For property and casualty insurers, the evidence component is often the most complex part. A single auto accident claim might include dashcam footage from two vehicles, body camera video from responding officers, photos of vehicle damage, a recorded statement from the policyholder, medical records, and a surveillance video from a nearby business. Managing all of that across email threads and file shares creates chaos.
The Insurance Information Institute reports that US property and casualty insurers processed over $780 billion in direct premiums written in 2024. Each premium dollar carries a claims investigation cost. When that investigation relies on manual evidence handling, costs climb and cycle times stretch.
The Evidence Volume Problem
Claims investigations have become more evidence-intensive over the past decade. Ring doorbells capture incidents. Smartphones record everything. Telematics data from connected vehicles provides second-by-second crash reconstruction. Adjusters who used to review a few photos and a written statement now face gigabytes of multimedia per claim.
Without a system designed for multimedia evidence management, adjusters spend more time searching for files than actually analyzing them. That delay adds days to claim resolution and increases the risk of missing fraudulent patterns across related claims.
Why Do Insurance Claims Investigations Need Centralized Evidence?
Centralized evidence management solves the fragmentation problem that slows down every stage of a claims investigation. When all evidence lives in one repository with consistent metadata, every authorized team member can find what they need without asking someone else to email a file.
Here's what centralization changes in practice:
Single source of truth per claim. Every video, document, photo, and audio recording is linked to a claim number. No more hunting through shared drives or individual inboxes.
Consistent metadata and tagging. Evidence is tagged with claim identifiers, dates, claimant names, and evidence types at upload. Search works across the entire repository.
Access controls by role. Adjusters see their assigned claims. Managers see team portfolios. External counsel gets limited, time-bound access to specific evidence. No one sees more than they should.
Audit trail from day one. Every upload, view, download, and share is logged with timestamps, user identity, and IP address. This record matters when claims go to litigation.
The National Association of Insurance Commissioners (NAIC) has emphasized data governance and evidence handling in its model regulations. Centralized systems make compliance audits straightforward because the evidence trail is already documented. For a deeper look at why logging matters, see our guide on why digital audit trails matter in evidence management.
How Does AI Accelerate Claims Evidence Review?
AI transforms claims evidence review from a manual, linear process into a searchable, prioritized workflow. Instead of watching every minute of a recorded statement, adjusters can search for specific topics, phrases, or objects across an entire evidence library.
Three AI capabilities matter most for claims processing.
Automatic Transcription and Search
Recorded policyholder statements are the backbone of most claims investigations. Transcribing these manually takes roughly four hours for every hour of audio. AI transcription handles the same work in minutes, producing searchable text that adjusters can query by keyword. For a broader look at how AI is reshaping the entire claims lifecycle, see our guide on AI claims processing automation.
When an adjuster suspects inconsistencies between a claimant's statement and the physical evidence, searching transcripts across multiple recordings takes seconds. That cross-referencing capability catches fraud patterns that manual review misses.
Object Detection in Visual Evidence
Photos and video from accident scenes, property damage claims, and surveillance feeds contain details that matter for claim decisions. AI object detection identifies vehicles, license plates, faces, and specific objects within visual evidence. An adjuster reviewing a property damage claim can search for specific items across hundreds of photos instead of scrolling through each one individually.
PII and PHI Detection
Claims evidence frequently contains sensitive personal information: Social Security numbers in documents, faces in surveillance footage, medical details in recorded statements. Before sharing evidence with third parties, legal teams, or regulators, that information needs redaction. AI-based detection identifies these elements automatically, flagging them for review or redacting them in bulk.
What Role Does Evidence Integrity Play in Claims Disputes?
When a denied claim goes to litigation or regulatory review, the insurer must prove that evidence wasn't altered after collection. Evidence integrity is the ability to demonstrate, with cryptographic proof, that a file hasn't been modified since it entered the system.
Two technical mechanisms make this possible:
Hash-based tamper detection. When evidence is uploaded, the system generates a SHA-256 hash, a unique digital fingerprint of the file. Any modification changes the hash, making tampering immediately detectable.
Write-once, read-many (WORM) storage. Critical evidence is stored in immutable storage. Even system administrators can't modify or delete it during the retention period.
These mechanisms create what courts and regulators recognize as a defensible chain of custody. The Federal Rules of Civil Procedure (FRCP) require parties to preserve electronically stored information (ESI) once litigation is reasonably anticipated. A system with built-in integrity controls meets that obligation automatically. To understand what happens when this chain breaks, read our analysis of broken chain of custody causes, consequences, and prevention.
For insurers, this matters every time a denied claim leads to a bad faith lawsuit. If the evidence trail is incomplete or the insurer can't prove files weren't altered, the legal exposure grows significantly. A strong integrity framework supports digital evidence admissibility in any proceeding.
How Should Insurers Handle Sensitive Data in Claims Evidence?
Every claims file contains information regulated under multiple frameworks. A single auto injury claim might include PHI (medical records under HIPAA), PII (driver's license numbers, Social Security numbers), and PCI data (payment card information for rental car charges). Sharing that evidence without proper redaction creates regulatory risk and potential liability. For a full breakdown of the regulatory landscape, see our guide on compliance standards for evidence handling.
Manual redaction is the bottleneck. An adjuster redacting a 30-minute recorded statement by hand, bleeping spoken names, addresses, and account numbers, might spend two to three hours on a single file. Multiply that across dozens of claims per adjuster per month, and the labor cost becomes enormous.
Automated Redaction Across Media Types
The most effective digital claims processing platforms handle redaction across all evidence types, not just documents:
Video redaction: Faces blurred or pixelated, license plates obscured, on-screen text redacted.
Audio redaction: Spoken PII muted or bleeped, including names, addresses, SSNs, and phone numbers.
Document redaction: Keyword-based and pattern-based redaction in PDFs and scanned documents, including handwritten text via OCR.
Image redaction: Faces, identifying features, and text in photos automatically detected and redacted.
This multi-format approach matters because claims evidence isn't just documents. The surveillance video, the recorded statement, and the medical PDF all need redaction before sharing with defense counsel or regulatory bodies.
How Does Secure Evidence Sharing Work in Multi-Party Claims?
Claims investigations involve multiple parties who need access to evidence at different stages. Adjusters, special investigations unit (SIU) analysts, defense counsel, independent medical examiners, and sometimes regulators all need to view specific evidence without seeing the entire claim file.
Email attachments are the default for most carriers. They're also the worst option for security. Once a file is emailed, the sender loses all control over who views it, copies it, or forwards it.
Controlled sharing replaces email attachments with managed access:
Time-limited access links. Evidence is shared via URLs that expire after a set period. Recipients can view but not download, or download with watermarks.
Per-recipient tracking. Each share link is unique to the recipient, creating an audit record of exactly who accessed what and when.
Role-based visibility. External counsel sees only the evidence relevant to their matter. SIU analysts see the full investigation file. Claimants see only what they've submitted.
Access reason provisioning. Before viewing sensitive evidence, users must state their reason for access, creating an additional compliance record.
For SIU teams investigating potential fraud, this controlled sharing model is essential. It prevents evidence leakage during active investigations while still enabling the collaboration that complex claims require. For more on building secure sharing workflows, see our best practices for secure digital evidence sharing.
How VIDIZMO DEMS Supports Digital Claims Processing
VIDIZMO DEMS (Digital Evidence Management System) brings these capabilities together in a single platform designed for evidence-intensive workflows. For insurance carriers, the platform addresses the specific challenges outlined above.
DEMS centralizes all claims evidence, including video, audio, documents, and images across 255+ supported formats, in a single repository with case-based organization. AI-powered transcription covers 82 languages with published accuracy benchmarks, turning recorded statements into searchable text. AI-assisted redaction handles PII, PCI, and PHI detection across all media types, replacing the manual redaction bottleneck with automated workflows.
Evidence integrity features include SHA-256 tamper detection and WORM-enabled storage, producing exportable chain-of-custody reports for any claim that reaches litigation. Role-based access controls, time-limited sharing links, and per-user tokenized URLs ensure evidence moves securely between claims teams and external parties.
For carriers ready to modernize their claims evidence workflows, the first step is evaluating how your current systems handle multimedia evidence at scale.
Request a free DEMS trial to see how centralized evidence management transforms your claims investigation process.
How Should You Evaluate a Digital Claims Processing Platform?
Not every evidence management system is built for insurance workflows. When evaluating platforms, focus on these criteria:
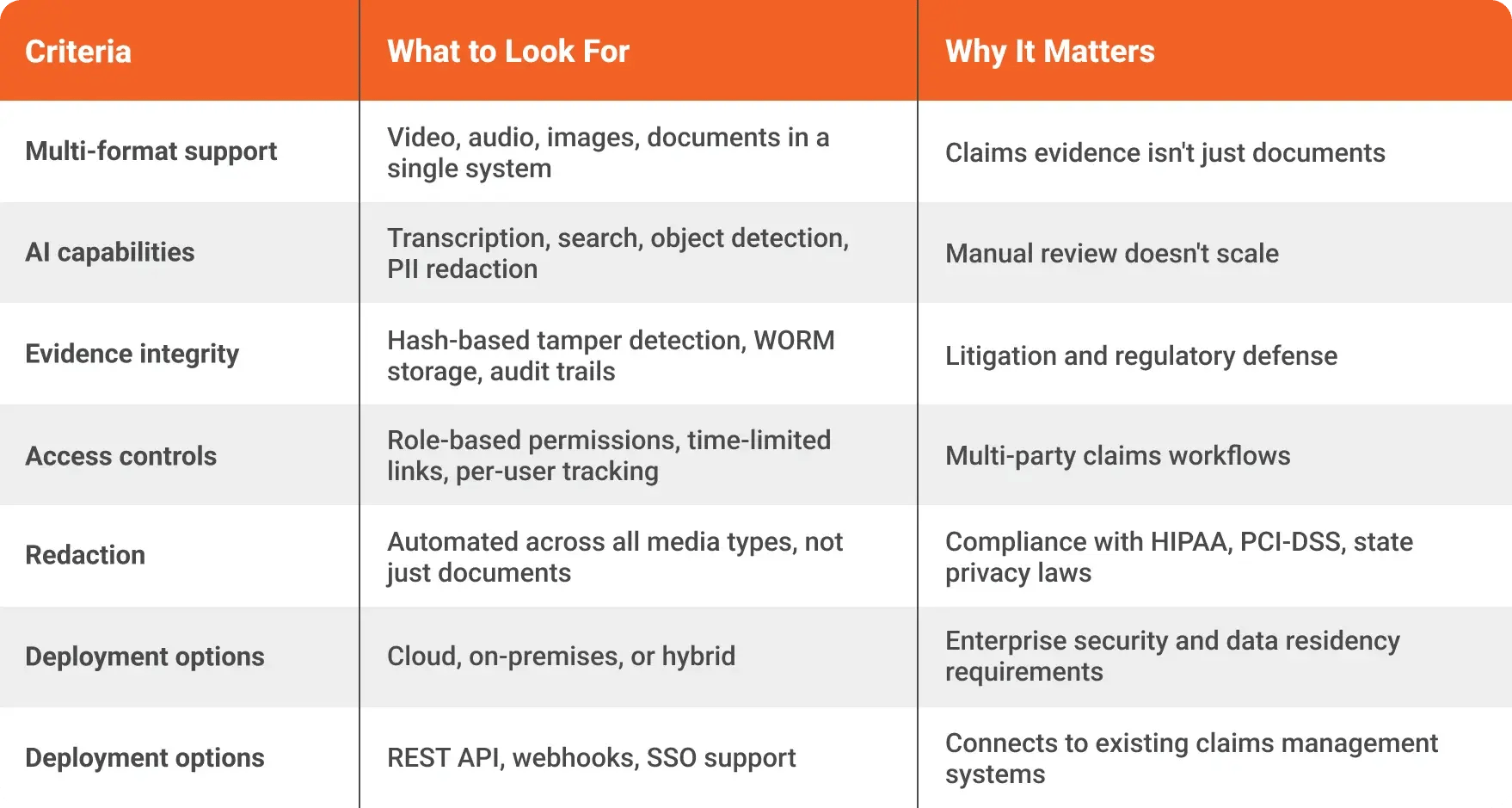
Carriers with strict data residency requirements should pay special attention to deployment flexibility. A platform that only offers public cloud won't work for insurers subject to state-level data handling regulations or those managing claims involving government entities.
People Also Ask
Digital claims processing is the management of insurance claims evidence and workflows through electronic systems rather than paper-based or manual methods. It includes digitizing evidence intake, using AI for evidence review and redaction, maintaining tamper-proof audit trails, and sharing evidence securely with authorized parties through controlled access links.
Digital systems enable cross-referencing evidence across multiple claims through AI-powered search and transcription. Adjusters can search recorded statements for specific phrases or inconsistencies, identify duplicate photos submitted across different claims, and flag patterns that manual review would miss. The Coalition Against Insurance Fraud estimates that fraud costs US insurers over $80 billion annually, making detection technology a high-ROI investment.
A capable platform manages all multimedia evidence types found in claims investigations: loss adjustment videos, recorded policyholder statements, surveillance footage, photographs of damage, medical records, police reports, telematics data, and supporting documents. VIDIZMO DEMS supports 255+ file formats across video, audio, images, and documents in a single repository.
AI-powered redaction automatically detects sensitive information across media types. For video, it identifies and blurs faces and license plates. For audio, it mutes spoken PII like names and Social Security numbers. For documents, it finds and redacts text patterns matching PII, PCI, and PHI data. This approach replaces manual redaction that can take hours per file with an automated workflow that handles bulk evidence in minutes.
Traditional claims handling relies on physical media, email attachments, and manual evidence review. Digital processing centralizes everything in a searchable repository with AI-powered analysis, automated redaction, and controlled sharing. McKinsey research shows digitized claims operations achieve 30 to 50 percent faster processing times while improving fraud detection accuracy.
Insurance claims evidence falls under multiple regulatory frameworks depending on content type: HIPAA for medical records, PCI-DSS for payment card data, state privacy laws for PII, and the Federal Rules of Civil Procedure for evidence preservation in litigation. A digital claims platform should support compliance through role-based access controls, audit logging, automated redaction, and configurable retention policies.
Yes. Modern evidence management platforms offer REST APIs, webhook integrations, and SSO support to connect with existing claims management, policy administration, and case management systems. This integration allows evidence to flow between systems without manual file transfers, maintaining the audit trail across platforms.
Conclusion
Digital claims processing isn't about moving from paper to PDF. The real transformation happens when insurers treat claims evidence as a managed, searchable, auditable asset rather than a collection of files scattered across inboxes and shared drives.
Centralized evidence management, AI-powered review, automated redaction, and controlled sharing cut investigation timelines while strengthening fraud detection and regulatory compliance.
About the Author
Rafay Muneer
Rafay Muneer is a Senior Product Marketing Strategist at VIDIZMO with deep expertise in data protection, AI redaction, and privacy compliance. He covers how public safety agencies, legal teams, and enterprise organizations build defensible, technology-driven approaches to sensitive data management.
Jump to
You May Also Like
These Related Stories

How AI and Automation Are Transforming Insurance Claims Processing

What Is Digital Claims Processing? Complete Guide for Insurance Carriers




No Comments Yet
Let us know what you think